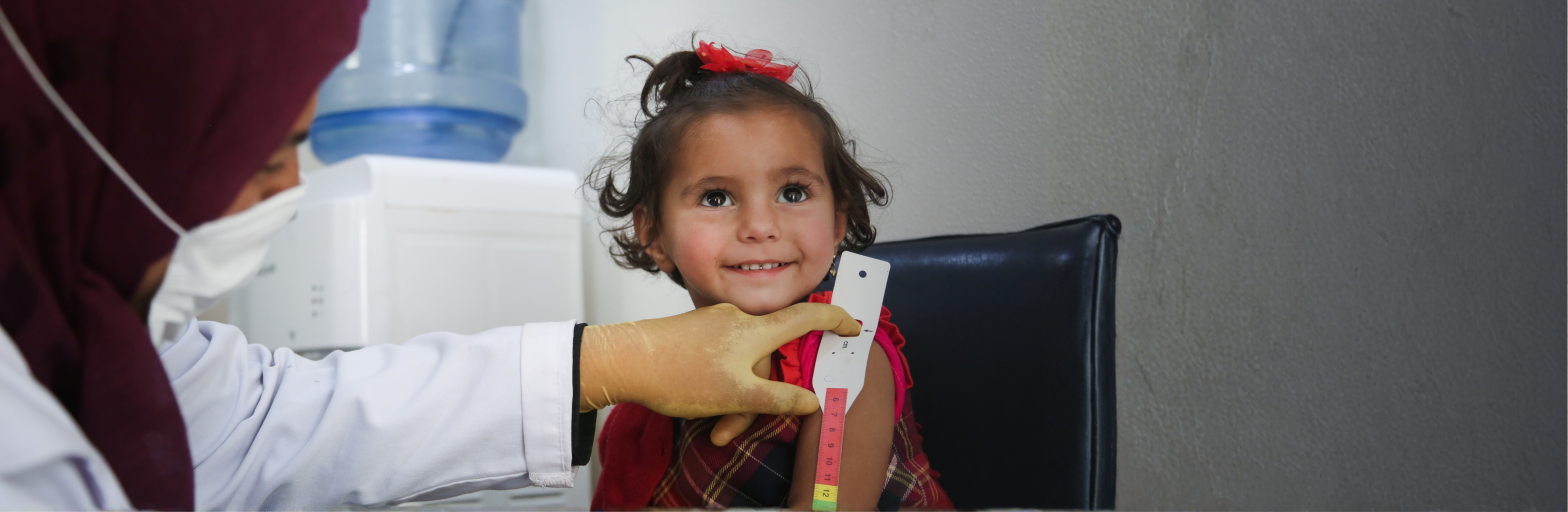
World Health Day 2026: Together...
This World Health Day, USCRI’s Refugee Health Services (RHS) recognizes the vital role of science and the communities that bring...
READ FULL STORY
By: Rosalind Ghafar Rogers, PhD, LMHC, Clinical Behavioral Health Subject Matter Expert
with USCRI’s Refugee Health Services in Arlington, VA
March is self-harm awareness month. Although less often talked about publicly, it is a common clinical problem that poses a significant public health concern. Research indicates that self-harm occurs in approximately 5% of adults, 17% of adolescents, and between 17% and 35% of college students in the U.S. (MHA, n.d.). Although the onset of self-harm can occur as early as 7-years-old, the average age of onset is usually 12 to 15 years of age. Self-harm exists in almost all countries and cultures and across all age groups and demographics.
Commonly referred to as self-injurious behavior and clinically termed non-suicidal self-injury (NSSI), self-harm is any form of self-destructive, non-suicidal, private behavior that deliberately inflicts physical harm on or mutilates one’s body to relieve or distract from emotional distress. To be clear, NSSI does not involve the conscious intent to die by suicide nor is it an attempt at attention-seeking. It is also important to note that NSSI is often habitual because it provides an outlet when other attempts at coping or tolerating distress have failed. NSSI can take many forms and can include cutting, picking, burning, pinching, biting, bruising, scratching, pulling hair, skin carving, ingesting harmful substances, head banging, or striking one’s head or other body part against a wall or floor. The arms, legs, chest, and stomach are the most frequently targeted parts of the body. NSSI mostly happens in private and is often done in a controlled manner or the same way each time.
Symptoms of NSSI include but are not limited to:
NSSI can be understood as a way to communicate or expel what cannot be spoken, expressed, or shared. Symbolically, the body or skin is the canvas and the cut, bruise, burn, or poison is the paint that illustrates the self-portrait or picture (Serani, 2022). Most individuals who engage in NSSI struggle to express their emotions or needs. Although they vary considerably, common reasons for engaging in NSSI include:
Although NSSI may provide temporary relief in the moment, it creates far more problems than it solves. Any short-term relief from self-harm is quickly followed by feelings of shame and/or guilt and the problems and/or feelings that triggered the self-harm remain unsolved. Engaging in NSSI prevents individuals from learning and using more effective strategies to address their issues. Because shame is often both a trigger and an outcome of NSSI, secrecy, social isolation, and loneliness are additional negative consequences. Along with the possibility for scarring and infections, each act of self-harm has the potential to be lethal due to accidents. Moreover, NSSI is a significant risk factor for the development of severe mental illness and is one of the strongest predictors of future self-harm and suicide (Gholamrezaei et al., 2023; Hedrick & Borschmann, 2023).
NSSI exists in almost all cultures and ethnicities, but prevalence rates, contributing factors, functions, and methods of NSSI may be different across cultures and contexts. Although studies in non-Western countries are limited compared Western countries, lifetime prevalence rates of NSSI have been reported among young adults in China (23%), Belgium (8%), India (21%), Turkey (15-33%), Mexico (17-19%), and the U.S. (12-23%) (Gandhi et al., 2021; Mannekote Thippaiah et al., 2021). Ethnic variations in the methods of NSSI have also been reported: cutting and scratching in Belgium and the U.S.; head banging and self-hitting in India; skin cutting, skin picking, and biting in Mexico; head banging and striking of the head or other body parts against a wall or floor in Turkey; and self-hitting, pinching, and hairpulling in China (Mannekote Thippaiah et al., 2021). Various risk factors have also been reported internationally: In China, risk factors of NSSI included restrictive weight control behaviors, poor perceived body image, and loss of face; in South Africa, relationship issues, unemployment, and rape; in Pakistan, marital status, interpersonal conflict, poverty, and marital disharmony; among youth in an Eastern cultural context, strict gender norms and practices, such as child or arranged marriages, overly high expectations by parents of children’s academic achievement, and stigma associated with mental health issues and NSSI; and self-immolation (setting fire to oneself) by women in developing countries and traditional societies as a form of protest against oppression, discrimination, abuse, and disenfranchisement (Chen et al., 2021; Mannekote Thippaiah et al., 2021; Nisavic et al., 2017).
In addition to cultural factors, migration has been identified as a risk factor for engaging in self-harming behaviors due to migrants’ and refugees’ higher vulnerability to various pre-, peri-, and post-migration trauma and stress, which also increases the risk of mental health issues. Although research is limited, studies have indicated higher prevalence rates of NSSI among migrants and refugees compared to host country populations (Baralla et al., 2021). Post-resettlement factors have also been linked to a higher potential for self-harm, as well as suicidal behavior, among migrants and refugees. Acculturation stress, discrimination and social marginalization, changes in social roles and socioeconomic status, language barriers, separation from family, and loss of a social network have all been identified as possible risk factors for NSSI (Basu et al., 2022). Factors associated with immigration processes and asylum processing procedures have also been linked to increased rates of NSSI among refugees and immigrants. For example, among asylum seekers in detention facilities in Australia, rates of NSSI were considerably higher compared to asylum seekers in community-based settings (Hedrick et al., 2019), and among children held in detention centers, there is a ten-fold increase in the incidence of self-harm (Hendrick & Borschmann, 2023). Among asylum seekers obligated to remain in a German reception center for up to 18 months after submitting their application, approximately 26% reported acute self-harming behavior, and of those who presented with suicidal ideation and behavior to psychiatric emergency services in Denmark, 61% were asylum seekers with asylum claims rejected (Posselt et al., 2020). Among young migrants and refugees, rates of NSSI are higher, with between 18% to 60% having self-harmed at some point since their migration (Basu et al., 2022; Donath et al., 2019).
Although there are universal aspects of NSSI that cut across all cultures and contexts, understanding the cultural and contextual factors that contribute to NSSI is becoming increasingly important, particularly at a time of heightened diversification and migration around the world.
If you are concerned about self-harming behaviors, support from a trained, compassionate healthcare provider or mental health professional is often the key to finding safe alternatives to self-harm and lasting change and healing.
If you are in a crisis or need support, please text HOME to 741741 to connect with a compassionate volunteer crisis counselor. To chat with a crisis counselor and/or to learn more about self-harm and how to recover, please visit the Crisis Text Line.
If you or someone you know may be experiencing a mental health crisis or contemplating suicide, please call the 24/7 National Suicide Prevention Lifeline at 988. In emergencies, call 911, or seek care from a local hospital emergency room or mental health provider.
References
Al-Sharifi, A., Krynicki, C. R., & Upthegrove, R. (2015). Self-harm and ethnicity: A systematic review. International Journal of Social Psychiatry, 61(6), 600-612.
Baralla, F., Ventura, M., Negay, N., Di Napoli, A., Petrelli, A., Mirisola, C., & Sarchiapone, M. (2021). Clinical Correlates of Deliberate Self-Harm Among Migrant Trauma-Affected Subgroups. Frontiers in Psychiatry, 12, 529361. https://doi.org/10.3389/fpsyt.2021.529361.
Basu, A., Boland, A., Witt, K., & Robinson, J. (2022). Suicidal behaviour, including ideation and self-harm, in young migrants: a systematic review. International Journal of Environmental Research and Public Health, 19(14), 8329.
Chen, X., Zhou, Y., Li, L., Hou, Y., Liu, D., Yang, X., & Zhang, X. (2021). Influential factors of non-suicidal self-injury in an Eastern cultural context: a qualitative study from the perspective of school mental health professionals. Frontiers in Psychiatry, 12, 681985. https://doi.org/10.3389/fpsyt.2021.681985.
Donath, C., Bergmann, M. C., Kliem, S., Hillemacher, T., & Baier, D. (2019). Epidemiology of suicidal ideation, suicide attempts, and direct self-injurious behavior in adolescents with a migration background: a representative study. BMC pediatrics, 19(1), 1-15.
Gholamrezaei, M., Heath, N. L., Pereira, L., De Stefano, J., & Böke, B. N. (2023). Nonsuicidal Self-Injury, Mental Health Service Use, and Cultural Perspectives Among Ethnically Diverse University Students. Canadian Journal of Community Mental Health, 42(1), 1-26.
Hedrick, K., Armstrong, G., Coffey, G., & Borschmann, R. (2019). Self-harm in the Australian asylum seeker population: a national records-based study. SSM – Population Health, 8, 100452.
Hedrick, K., & Borschmann, R. (2023). Self-harm among unaccompanied asylum seekers and refugee minors: protocol for a global systematic review of prevalence, methods and characteristics. BMJ open, 13(6), e069237.
Mannekote Thippaiah, S., Shankarapura Nanjappa, M., Gude, J. G., Voyiaziakis, E., Patwa, S., Birur, B., & Pandurangi, A. (2021). Non-suicidal self-injury in developing countries: a review. International Journal of Social Psychiatry, 67(5), 472-482. https://doi.org/10.1177/0020764020943627.
Mental Health America (MHA). (n.d.). Self-injury (cutting, self-harm, or self-mutilation). https://www.mhanational.org/conditions/self-injury-cutting-self-harm-or-self-mutilation
Posselt, M., McIntyre, H., Ngcanga, M., Lines, T., & Procter, N. (2020). The mental health status of asylum seekers in middle-to high-income countries: a synthesis of current global evidence. British Medical Bulletin, 134(1), 4-20.
Serani, D. (2022). March is self-injury awareness month. Psychology Today. https://www.psychologytoday.com/us/blog/two-takes-depression/202203/march-is-self-injury-awareness-month

This World Health Day, USCRI’s Refugee Health Services (RHS) recognizes the vital role of science and the communities that bring...
READ FULL STORY
By: Rosalind Ghafar Rogers, PhD, LMHC, Clinical Behavioral Health Subject Matter Expert with USCRI’s Refugee Health Services in Arlington, VA...
READ FULL STORY
By: Rosalind Ghafar Rogers, PhD, LMHC, Clinical Behavioral Health Subject Matter Expert with USCRI’s Refugee Health Services in Arlington, VA...
READ FULL STORY